When the cat’s liver fails there are several conditions that we look to as the most common causes:
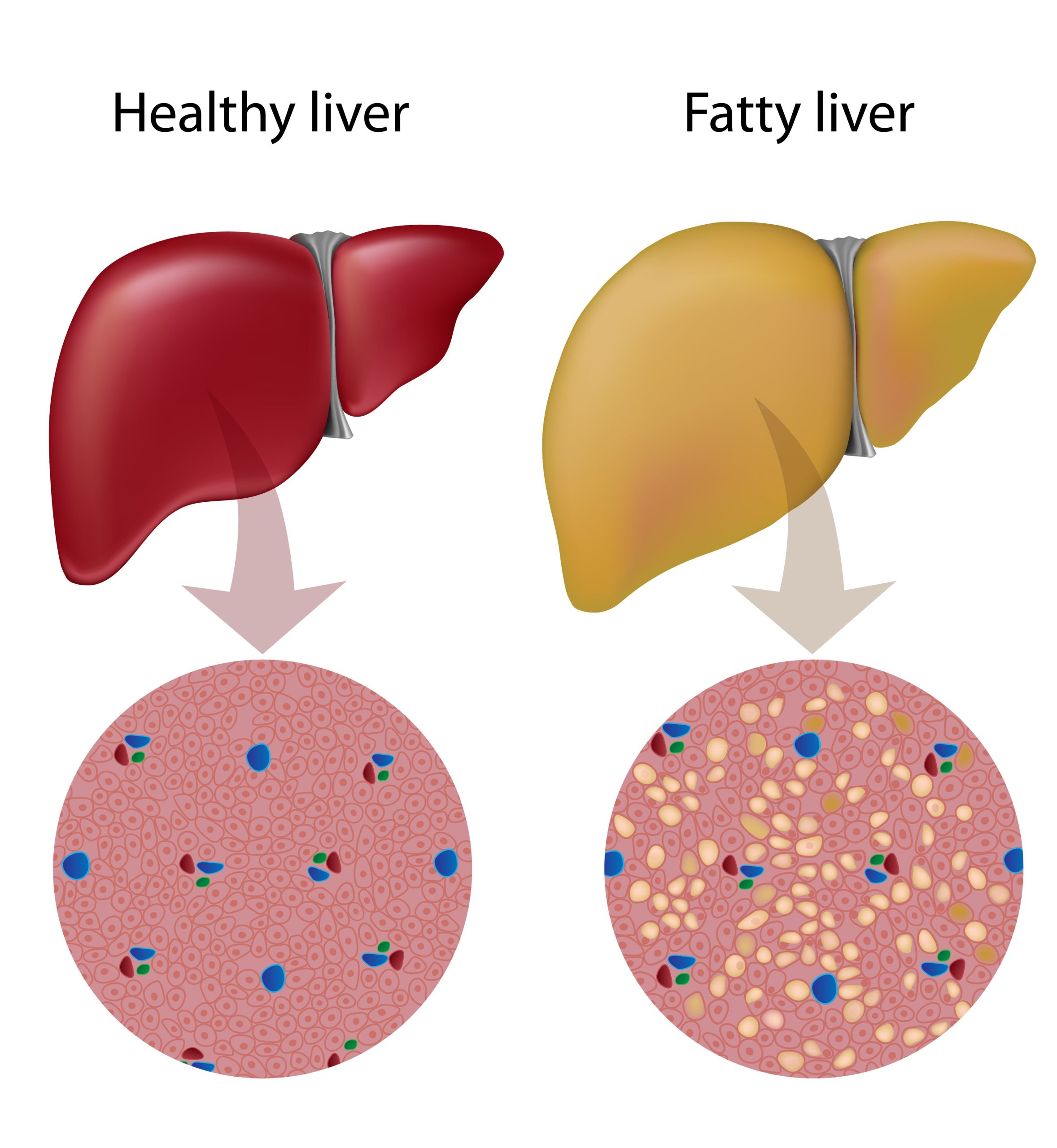
- Hepatic Lipidosis (“fatty liver”)
- Lymphoma (a type of cancer)
- Cholangiohepatits/cholangitis
- Feline Infectious Peritonitis
- Necrosis (usually from drugs or toxins)
- Misc. Cancers
- Cholangiohepatitis can mean either inflammation of the liver or bile ducts or both.
Bile has several functions. It emulsifies the fat in our diets so that we can absorb it
into our bodies. It also serves as a medium to dump toxins that the liver has
removed from our bodies and processed so they cannot be reabsorbed. This is a
fine system but problems can occur when the bacteria that live in the small intestine
venture up the bile duct and invade the liver, which is normally sterile
(free of bacteria). Inflammation results and the liver can fail.
However, DEA 1 negative dogs aren’t truly “universal donors” because a dog may be positive for another blood type that might cause an issue.
To make sure there won’t be a serious immune reaction to any of a donor dog’s blood types, the veterinarian will do another test called “crossmatching.” This test checks the overall compatibility of donor and recipient blood.
After confirming DEA 1 blood type and running a crossmatching test, a veterinarian can typically determine which type of blood will be the most successful for the dog receiving the transfusion.
Symptoms
The average cat with this condition is a young adult male with fairly sudden onset of vomiting, diarrhea, appetite loss, and listlessness. Often there is a fever and abdominal pain. Blood tests are typical of inflammation and liver disease with elevations in liver enzymes, white blood cell count, and bilibrubin
Diagnosis
Biochemistry blood test can be done to check on the liver enzymes leverl. Ultrasound or similar imaging helps sort out which is which but to really get the answer, a tissue sample of some kind is needed. An aspirate or needle biopsy involves withdrawing a small sample through a needle. This method can detect lymphoma and lipidosis readily but cholangiohepatitis will require an actual biopsy which is more invasive and requires a larger tissue sample.
Treatment
The cat in liver failure will require hospitalization, fluid therapy, and some kind of nutritional support (force-feeding, tube feeding, syringe feeding of a liquid diet or whatever is necessary) regardless of the cause of the liver disease. Antibiotics Antibiotics are helpful in any liver failure case as they help reduce the intestinal bacterial populations (any noxious substances they produce are normally detoxified by the healthy liver but a sick liver will not be so efficient). Antibiotics also clear the liver of invading bacteria, which is what cholangiohepatitis is all about. Expect the cat to require 1-3 months of antibiotics after recovery. Choleretics A choleretic is a medication that makes bile more liquid so that it can flow smoothly without sludging. Flow of bile in the proper direction helps remove not only the toxins the liver is trying to remove in bile but also helps prevent bacteria from “swimming upstream” towards the liver tissue. The chief choleretic prescribed for animals is Ursodiol. A cat may well be on this medication for life after an episode of cholangiohepatitis. SAMe This nutritional medicine has gained tremendous popularity in therapy for all liver diseases and should probably not be left out here. SAMe stands for S-adenosylmethionine. It has several desirable functions but mostly it is an antioxidant, protecting the sick liver cells from the toxins they have absorbed and normally would be excreting in bile.

